November is Prematurity Awareness Month, with World Prematurity Day observed on November 17th, and helps to raise awareness of preterm births and the concerns of preterm babies and their families worldwide. Having a baby is a life-changing, amazing experience, but for some, especially moms who have or had babies in the Neonatal Intensive Care Unit (NICU), it can be a stressful, traumatizing, and frightening time. While research shows 10-15% of women who give birth are diagnosed with Post-Partum Depression (PDD), the number is much higher with NICU parents—almost to 40% and even higher if you include Perinatal Mood and Anxiety Disorders (PMAD). At Saint Barnabas Medical Center in Livingston, an affiliate of RWJBarnabas Health, the staff and programs ensure every mom and baby in the NICU has the support and attention they need. Their innovative program, The NICU Buddy Program, pairs parents with other parents who’ve been there—providing the reassurance and hope that only a parent who’s been in those shoes can provide. And because of the exceptional care and supportive environment, parents can find the help they need, especially if they’re experiencing PDD or PMAD. Read on for one mother’s story and learn more about the NICU baby and parent care at Saint Barnabas Medical Center, an affiliate of RWJBarnabas Health, and how they are supporting families during a difficult time.
Become an NJMOM Insider! For all the best things to do with your family around New Jersey, be sure to sign up for our weekly newsletter delivered right to your inbox each week, and don’t forget to tag your photos #NJMOM and @njmom for a chance to be featured on our social media.
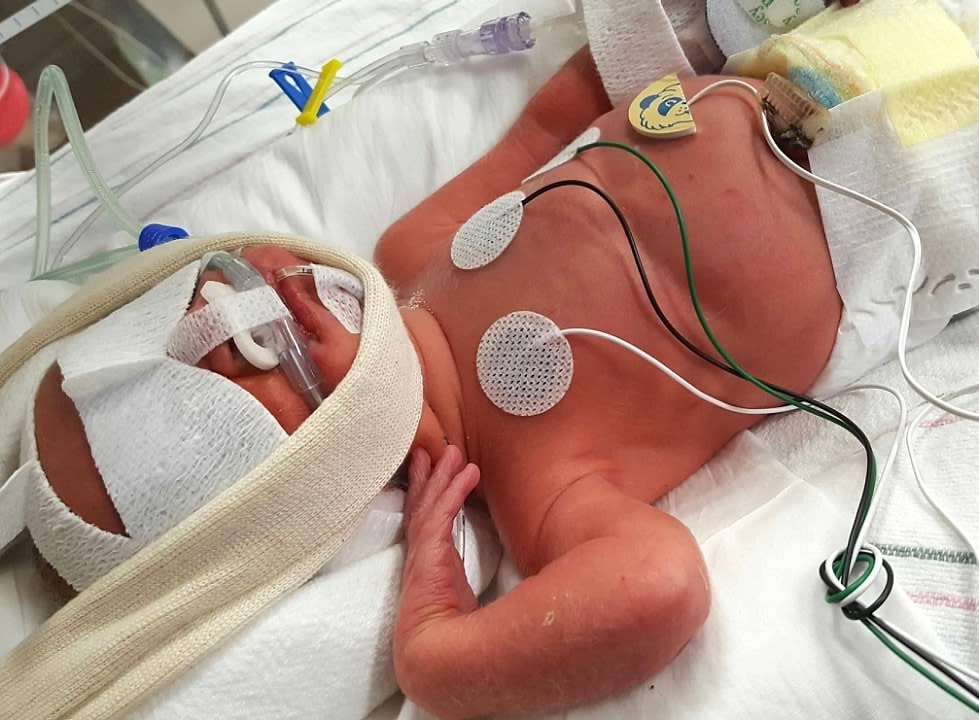
“The NICU staff will always hold a special place in our hearts, and we cherish their dedication to caring for premature and sick babies,” says Krystal.
A Person Who’s Been There: Krystal’s Story
On the morning of May 7, 2014, I woke with lower back pain thinking it was normal symptoms of pregnancy. I went about my morning routine and commuted into NYC. But, once I got to the subway, I knew going to work was the wrong decision. I had shooting pains down my legs and worse lower back pain. I was in so much discomfort that I only lasted a short time at work before deciding to head home. As I got up to leave, my water broke. I called my OB/GYN in NJ who said I needed to go to the nearest hospital for treatment. I was in denial because, at only 28+6 weeks pregnant, I did not think I was going to have my baby, but I was. Thankfully, the hospital I chose had a level III NICU but still to this day I wish I could have delivered at Saint Barnabas Medical Center (SBMC).
When I got to the hospital, I was 4 cm dilated and my water broke. I was put on magnesium, given steroids, and eventually an epidural for back labor. I stayed like that overnight but by the next morning, I was almost 10 cm dilated and knew my baby boy was coming. Indeed, Jaxon arrived on May 8, 2014, at 11:10 am, weighing 3 pounds, 11 ounces; he was 29 weeks exactly. He was rushed directly to the NICU. I did not hear him cry, I did not get to see him until hours later, and when the shock of delivering a baby 11 weeks early wore off, the hardships of being a NICU mom began to set in.
The first time I saw him, I did not know what to think or how to feel. I was numb and only remember feeling sorrow and fear. I loved him beyond measure and was overjoyed to meet him, but this was far from how I expected us to meet. I had barely begun my third trimester and didn’t even have my baby shower yet, but there I was, staring at my tiny baby boy, intubated, and covered in wires. It hurt so badly to see him like that, and it broke my heart knowing that I was the main cause of his early arrival due to my uterine anomaly.
By day 4 of life, Jaxon had his first head ultrasound. Being new parents and new NICU parents, we did not know all the terms, the risks, or the procedures being done. We went along with what the doctors said and hoped he was in the best hands. Call it a mother’s instinct, but I knew the second I entered the NICU that day that something was not right with my baby, and I was right. A neonatologist came to speak to my husband and me in the hallway to let us know that Jaxon had a grade 2, almost 3, bilateral brain bleed or as he said an intraventricular hemorrhage (IVH). I remember him saying, “We hope it resolves on its own and does not progress.” I also remember him saying things like hydrocephalus, and the possibility of cerebral palsy, mental retardation, developmental delays, motor and eating problems, speech, and vision issues. This was the exact moment when the trauma of my delivery, met the post-traumatic stress I was experiencing, and eventually met the postpartum anxiety. This is the moment where bonding with my new baby became hard because I feared losing him more than having him.
By day 7, Jaxon’s diagnosis worsened and his IVH progressed to grade 3. He was starting to develop hydrocephalus. I was never comfortable having Jaxon in NY so once his diagnosis worsened, it was time to have him transferred. I called Saint Barnabas Medical Center (SBMC) in Livingston, NJ, on a Thursday and by Tuesday, Dr. Kamtorn, a neonatal specialist at Saint Barnabas Medical Center had arranged to have Jaxon transported via ambulance from NY to NJ. A huge weight was lifted off my shoulders when the neonatologist, two nurses, and the respiratory specialist from SBMC arrived in NY to transport Jaxon. Once he was at SBMC, the neonatologist reviewed his records and ran his own set of tests and scans, but the results stayed the same as in NY. Doctors tried spinal taps three different times to relieve some of the intracranial pressure and his hydrocephalus but, unfortunately, it did not. The NY hospital told us that a shunt in his brain would not be considered until Jaxon was 6-9 months of age, but Dr. Kamtorn and a pediatric neurosurgeon at SBMC felt differently. They suggested that a shunt should be considered as soon as possible to relieve pressure and lessen the risk of brain damage. I am so thankful they persisted, and we listened. Within one week of arriving at SBMC, Jaxon was taken into surgery to have his VP shunt placed. I trusted the staff at SBMC’s NICU fully and put my child’s life in their hands. The surgery was a success. A blood transfusion assisted him in bouncing back after surgery and by the next week, we were bottle-feeding a brave, resilient boy. Learning to feed was a long process for him. It took him six frustrating weeks, but I learned patience and began the process of healing from my trauma. After 76 days in the NICU, Jaxon came home one day before his due date. He met his milestones between his actual and adjusted age and seemed to defy all the odds. He’s an amazing, spirited, inventive, and very creative boy; you’d never know the challenges he has overcome in his 7 years.
After being home with Jaxon I remember thinking I would only have one child. I was scared to try again because I feared going through the NICU a second time. But, when Jaxon was 15 months old, we were blessed with our second planned pregnancy. Doctors said “every pregnancy is different” but for me, that was not true. Weston arrived via c-section on April 17, 2016, at 29+1 weeks, weighing in at 3 pounds, 15 ounces. The doctors tried everything but carrying a baby closer to term did not seem possible for me. Jaxon and Weston’s birth timing and weight were almost the same, but they had very different journeys. Much of my trauma from Jaxon’s birth was due to him being born at an unknown hospital, with unknown doctors. Weston was born in the trusted hands of my NJ OB/GYN and with the SBMC NICU team waiting to tend to his every need. Weston did not need intubation at birth and was a champion feeder, but he faced his own challenges. He developed IVH grade one, had a protein intolerance, severe reflux, and had many apnea episodes. There were countless times I would watch his oxygen saturation plummet and his skin turn blue. Weston’s nurses would compassionately talk me through every frightening moment and remind my little guy to breathe. With time, Weston grew out of most of his apnea problems, but he did come home on an apnea monitor. He was discharged from the NICU after 65 days and just like the fighter who came before him, he conquered every challenge thrown at him with a giggle and a smile. He wears his heart on his sleeve and is such a funny, inquisitive, and bubbly, little boy.
Today, Jaxon and Weston are happy, healthy, and thriving boys who are growing out of shoes faster than Amazon prime can deliver! We are beyond thankful for the incredible care we received at SBMC’s NICU. The NICU staff will always hold a special place in our hearts, and we cherish their dedication to caring for premature and sick babies.
Like me, if you feel you have Post-Traumatic Stress Disorder (PTSD), Post-Partum Anxiety, or any mental health-related concern, seek counseling and seek it as soon as you can. Mental health is critical after going through a journey like the NICU. And having a parental support network, as we had at Saint Barnabas Medical Center NICU, who can help you from the standpoint of experience and training, is not only beneficial but also crucial. You have a built-in warrior to hold your hand while you fight your battles. You can speak to this person as much or as little as you want and communicate in any way you are comfortable with—text, calls, or in person. You get out of this what you need, and you learn so much from someone who can personally relate to what you are going through. Having a caring person to help you during the process is huge because the NICU can feel isolating and overwhelming. Proudly, I became a parent buddy to help and support other NICU parents the same way that my buddy helped and supported me.

Jaxon and Weston are happy, healthy, thriving boys.
How The NICU Buddy Program at Saint Barnabas Medical Center Gives Parents Hope
The NICU Buddy Program at Saint Barnabas Medical Center has been helping NICU parents for over 13 years. According to Haley Hirschmann, NICU Family Advisory Council Coordinator, NICU Buddy Program Coordinator, Saint Barnabas Medical Center NICU, “Each parent who becomes a hospital volunteer must be a graduate of the NICU and take a four-hour training course. The buddy program has most often been utilized by longer-stay NICU parents who often have very sick or tiny babies known as micro-preemies, born less than 26 weeks gestation or less than 1 3/4 pounds and are in the hospital at least 10 weeks or more.”
Because NICU Buddy Program parents have had a similar experience, they can often provide exceptional support and information that only another parent who has been there can. And while shorter stay parents also find the program helpful, the parents who are in the NICU for an extended period find it highly beneficial, a lifeboat when they feel they are drowning. “The program is opt-in for patients, and when they do sign up, I match current NICU parents with trained graduate volunteer parents active in our system, who may also have had the same diagnosis. It gives the families hope,” says Hirschmann. For Krystal, her experience with Jaxon led her to find a buddy in the Buddy Program, and through her experience with Weston, she became more active as a volunteer to help others in a similar situation.

“Both my boys are growing and thriving. Know that it does get brighter, and there are plenty of better days ahead,” says Krystal.
Here’s Where NICU Parents Can Get Help From RWJBarnabas Health
The NICU can be a very stressful place, and the sights, sounds, and fear in the NICU can affect parents for months after. So, are all NICU parents doomed to suffer from anxiety, depression, and Post-Traumatic Stress Disorder? Not always, and if you do feel this way, these problems are treatable. You don’t need to suffer alone—tell someone about your feelings. If you feel like you are going crazy, a familiar feeling most NICU parents describe, it’s best to share it with your OB/GYN. Be honest with them about how you feel (you will not be telling them anything they have not heard before). Plus, they will be ready to help you decide if you need a referral to a therapist to talk more or a short-term trial on medication. If you are more comfortable, talk to your “regular” doctor or internist, as they can also be a great resource.
It also can be helpful to talk to other people who have had experiences similar to yours. To pair moms with similar experiences and feelings, the hospital holds a psychologist-led Mommies Mood group (virtually at this time). Group facilitator Dr. Lauren Meisels says NICU parents often don’t come to the group until later on after the baby has come home from the hospital. “NICU parents often seem to be in “survival mode” until that point. They don’t become concerned until they are home with the baby and still feel depressed or anxious. They realize they need someone to help them through it. The group format creates a wonderful healing environment where attendees can share their similar feelings and worries without judgment,” she adds. Though it may seem difficult to make self-care a priority for you and your baby, it’s a necessity in maintaining your mental health and healing from the NICU. This means eating well, getting as much sleep as possible, and asking others to help you with meals or groceries if you are not up to it. You may also find taking walks, getting fresh air, praying, and meditating can alleviate your stress. And with the right support, you will get through it. While Krystal’s experience was traumatic, she’s seen the other side. Krystal is now a trained parent buddy and lends support to other NICU parents through the Buddy Program. “Both my boys are growing and thriving. Know that it does get brighter, and there are plenty of better days ahead. You will see the rainbow through the storm clouds—I have with extended support and help, and it’s only better from here.”
For more information about the NICU Buddy Program at Saint Barnabas Medical Center, an affiliate of RWJBarnabas Health, email Hayley.Hirschmann@rwjbh.org. For more information or to register for Mommies Mood Group, held Fridays from 11:00 am to 12:30 pm, contact Dr. Lauren Meisels at 973-322-5360 or lmeisels@icloud.com.
This post is sponsored by RWJBarnabas Health to help make every NJ mom and her family their healthiest.










